Maximize Your Stack




STUDY DESIGN
Randomized Double-Blind Controlled Study
Author Information Tatiana Moro, Grant Tinsley, Antonino Bianco, Giuseppe Marcolin, Quirico Francesco Pacelli, Giuseppe Battaglia, Antonio Palma, Paulo Gentil, Marco Neri and, Antonio Paoli Department of Biomedical Sciences, University of Padova, Padua, Italy. Department of Kinesiology & Sport Management, Texas Tech University, Lubbock, TX, USA. Sport and Exercise Sciences Research Unit, University of Palermo, Palermo, Italy. College of Physical Education and Dance, Federal University of Goias, Goiania, Brazil. Italian Fitness Federation, Ravenna, Italy. Department of Biomedical Sciences, University of Padova, Padua, Italy
BACKGROUND
Intermittent fasting (IF) is an increasingly popular dietary approach used for weight loss and overall health. While there is an increasing body of evidence demonstrating beneficial effects of IF on blood lipids and other health outcomes in the overweight and obese, limited data are available about the effect of IF in athletes. Thus, the present study sought to investigate the effects of a modified IF protocol (i.e. time-restricted feeding) during resistance training in healthy resistance-trained males.
METHODS
Thirty-four resistance-trained males were randomly assigned to time-restricted feeding (TRF) or normal diet group (ND). TRF subjects consumed 100 % of their energy needs in an 8-h period of time each day, with their caloric intake divided into three meals consumed at 1 p.m., 4 p.m., and 8 p.m. The remaining 16 h per 24-h period made up the fasting period. Subjects in the ND group consumed 100 % of their energy needs divided into three meals consumed at 8 a.m., 1 p.m., and 8 p.m. Groups were matched for kilocalories consumed and macronutrient distribution (TRF 2826 ± 412.3 kcal/day, carbohydrates 53.2 ± 1.4 %, fat 24.7 ± 3.1 %, protein 22.1 ± 2.6 %, ND 3007 ± 444.7 kcal/day, carbohydrates 54.7 ± 2.2 %, fat 23.9 ± 3.5 %, protein 21.4 ± 1.8). Subjects were tested before and after 8 weeks of the assigned diet and standardized resistance-training program. Fat mass and fat-free mass were assessed by dual-energy x-ray absorptiometry and muscle area of the thigh and arm were measured using an anthropometric system. Total and free testosterone, insulin-like growth factor 1, blood glucose, insulin, adiponectin, leptin, triiodothyronine, thyroid stimulating hormone, interleukin-6, interleukin-1β, tumor necrosis factor α, total cholesterol, high-density lipoprotein cholesterol, low-density lipoprotein cholesterol, and triglycerides were measured. Bench press and leg press maximal strength, resting energy expenditure, and respiratory ratio were also tested.
RESULTS
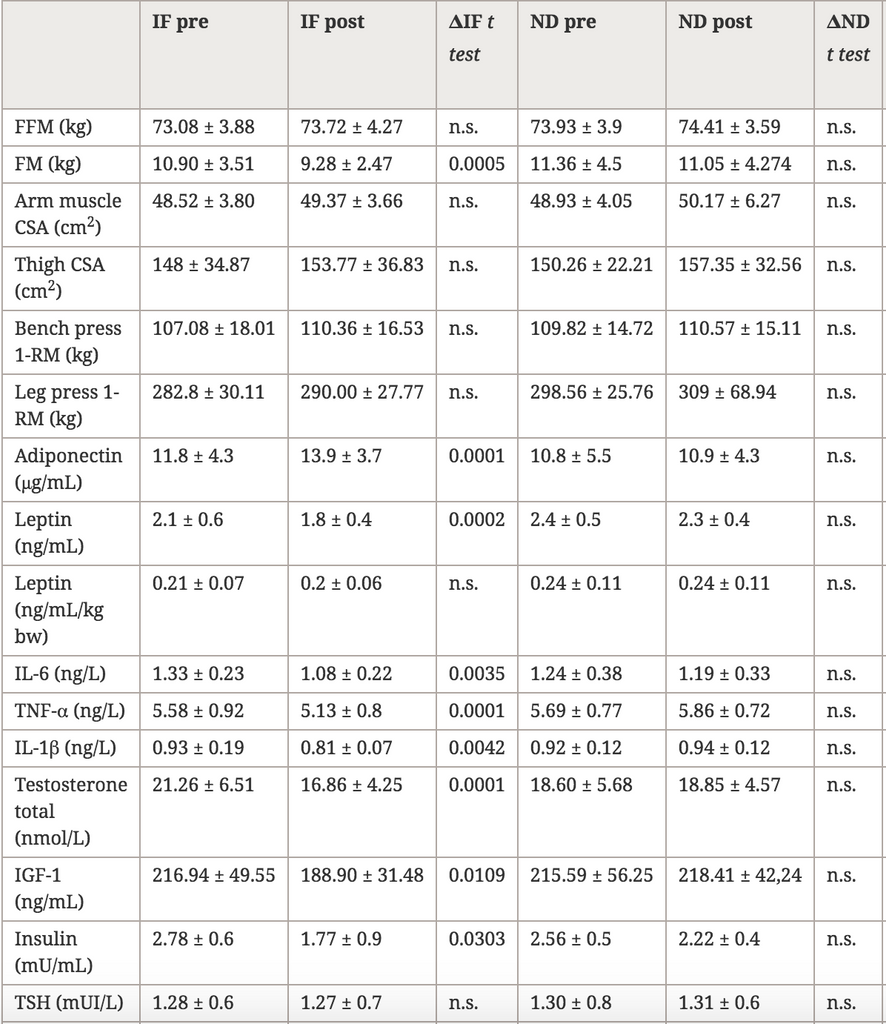
After 8 weeks, the 2 Way ANOVA (Time * Diet interaction) showed a decrease in fat mass in TRF compared to ND (p = 0.0448), while fat-free mass, muscle area of the arm and thigh, and maximal strength were maintained in both groups. Testosterone and insulin-like growth factor 1 decreased significantly in TRF, with no changes in ND (p = 0.0476; p = 0.0397). Adiponectin increased (p = 0.0000) in TRF while total leptin decreased (p = 0.0001), although not when adjusted for fat mass. Triiodothyronine decreased in TRF, but no significant changes were detected in thyroid-stimulating hormone, total cholesterol, high-density lipoprotein, low-density lipoprotein, or triglycerides. Resting energy expenditure was unchanged, but a significant decrease in respiratory ratio was observed in the TRF group.
CONCLUSIONS
Our results suggest that an intermittent fasting program in which all calories are consumed in an 8-h window each day, in conjunction with resistance training, could improve some health-related biomarkers, decrease fat mass, and maintain muscle mass in resistance-trained males.
- Trepanowski JF, Bloomer RJ. The impact of religious fasting on human health. Nutr J. 2010;9:57.View ArticlePubMedPubMed CentralGoogle Scholar
- Longo VD, Mattson MP. Fasting: molecular mechanisms and clinical applications. Cell Metab. 2014;19:181–92.View ArticlePubMedPubMed CentralGoogle Scholar
- Barnosky AR, Hoddy KK, Unterman TG, Varady KA. Intermittent fasting vs daily calorie restriction for type 2 diabetes prevention: a review of human findings. Transl Res. 2014;164:302–11.View ArticlePubMedGoogle Scholar
- Alkandari JR, Maughan RJ, Roky R, Aziz AR, Karli U. The implications of Ramadan fasting for human health and well-being. J Sports Sci. 2012;30(Suppl 1):S9–19.View ArticlePubMedGoogle Scholar
- Azizi F. Islamic fasting and health. Ann Nutr Metab. 2010;56:273–82.View ArticlePubMedGoogle Scholar
- Emami-Naini A, Roomizadeh P, Baradaran A, Abedini A, Abtahi M. Ramadan fasting and patients with renal diseases: a mini review of the literature. J Res Med Sci. 2013;18:711–6.PubMedPubMed CentralGoogle Scholar
- Faris MA, Kacimi S, Al-Kurd RA, Fararjeh MA, Bustanji YK, Mohammad MK, Salem ML. Intermittent fasting during Ramadan attenuates proinflammatory cytokines and immune cells in healthy subjects. Nutr Res. 2012;32:947–55.View ArticlePubMedGoogle Scholar
- Salim I, Al Suwaidi J, Ghadban W, Alkilani H, Salam AM. Impact of religious Ramadan fasting on cardiovascular disease: a systematic review of the literature. Curr Med Res Opin. 2013;29:343–54.View ArticlePubMedGoogle Scholar
- Aziz AR, Chia MY, Low CY, Slater GJ, Png W, Teh KC. Conducting an acute intense interval exercise session during the Ramadan fasting month: what is the optimal time of the day? Chronobiol Int. 2012;29:1139–50.View ArticlePubMedGoogle Scholar
- Bouhlel E, Salhi Z, Bouhlel H, Mdella S, Amamou A, Zaouali M, Mercier J, Bigard X, Tabka Z, Zbidi A, Shephard RJ. Effect of Ramadan fasting on fuel oxidation during exercise in trained male rugby players. Diabetes Metab. 2006;32:617–24.View ArticlePubMedGoogle Scholar
- Bouhlel E, Zaouali M, Miled A, Tabka Z, Bigard X, Shephard R. Ramadan fasting and the GH/IGF-1 axis of trained men during submaximal exercise. Ann Nutr Metab. 2008;52:261–6.View ArticlePubMedGoogle Scholar
- Burke LM, King C. Ramadan fasting and the goals of sports nutrition around exercise. J Sports Sci. 2012;30(Suppl 1):S21–31.View ArticlePubMedGoogle Scholar
- Chaouachi A, Leiper JB, Chtourou H, Aziz AR, Chamari K. The effects of Ramadan intermittent fasting on athletic performance: recommendations for the maintenance of physical fitness. J Sports Sci. 2012;30(Suppl 1):S53–73.View ArticlePubMedGoogle Scholar
- Javad Fallah S. Ramadan fasting and exercise performance. Asian J Sports Med. 2010;1:130.View ArticlePubMedPubMed CentralGoogle Scholar
- Stannard SR. Ramadan and Its Effect on Fuel Selection during Exercise and Following Exercise Training. Asian J Sports Med. 2011;2:127–33.View ArticlePubMedPubMed CentralGoogle Scholar
- Stannard SR, Thompson MW. The effect of participation in Ramadan on substrate selection during submaximal cycling exercise. J Sci Med Sport. 2008;11:510–7.View ArticlePubMedGoogle Scholar
- Bhutani S, Klempel MC, Kroeger CM, Trepanowski JF, Varady KA. Alternate day fasting and endurance exercise combine to reduce body weight and favorably alter plasma lipids in obese humans. Obesity. 2013;21:1370–9.View ArticlePubMedGoogle Scholar
- Klempel MC, Kroeger CM, Bhutani S, Trepanowski JF, Varady KA. Intermittent fasting combined with calorie restriction is effective for weight loss and cardio-protection in obese women. Nutr J. 2012;11:98.View ArticlePubMedPubMed CentralGoogle Scholar
- Klempel MC, Kroeger CM, Varady KA. Alternate day fasting increases LDL particle size independently of dietary fat content in obese humans. Eur J Clin Nutr. 2013;67:783–5.View ArticlePubMedGoogle Scholar
- Varady KA, Bhutani S, Klempel MC, Lamarche B. Improvements in LDL particle size and distribution by short-term alternate day modified fasting in obese adults. Br J Nutr. 2011;105:580–3.View ArticlePubMedGoogle Scholar
- Varady KA, Hellerstein MK. Alternate-day fasting and chronic disease prevention: a review of human and animal trials. Am J Clin Nutr. 2007;86:7–13.PubMedGoogle Scholar
- Tinsley GM, La Bounty PM. Effects of intermittent fasting on body composition and clinical health markers in humans. Nutr Rev. 2015;73:661–74.View ArticlePubMedGoogle Scholar
- Varady KA, Bhutani S, Church EC, Klempel MC. Short-term modified alternate-day fasting: a novel dietary strategy for weight loss and cardioprotection in obese adults. Am J Clin Nutr. 2009;90:1138–43.View ArticlePubMedGoogle Scholar
- Ziegler DR, Ribeiro LC, Hagenn M, Siqueira IR, Araujo E, Torres IL, Gottfried C, Netto CA, Goncalves CA. Ketogenic diet increases glutathione peroxidase activity in rat hippocampus. Neurochem Res. 2003;28:1793–7.View ArticlePubMedGoogle Scholar
- Paoli A, Bianco A, Grimaldi KA, Lodi A, Bosco G. Long term successful weight loss with a combination biphasic ketogenic mediterranean diet and mediterranean diet maintenance protocol. Nutrients. 2013;5:5205–17.View ArticlePubMedPubMed CentralGoogle Scholar
- Paoli A, Grimaldi K, Bianco A, Lodi A, Cenci L, Parmagnani A. Medium term effects of a ketogenic diet and a Mediterranean diet on resting energy expenditure and respiratory ratio. BMC Proc. 2012;6:P37.View ArticlePubMed CentralGoogle Scholar
- Anson RM, Guo Z, de Cabo R, Iyun T, Rios M, Hagepanos A, Ingram DK, Lane MA, Mattson MP. Intermittent fasting dissociates beneficial effects of dietary restriction on glucose metabolism and neuronal resistance to injury from calorie intake. Proc Natl Acad Sci USA. 2003;100:6216–20.View ArticlePubMedPubMed CentralGoogle Scholar
- Alirezaei M, Kemball CC, Flynn CT, Wood MR, Whitton JL, Kiosses WB. Short-term fasting induces profound neuronal autophagy. Autophagy. 2010;6:702–10.View ArticlePubMedPubMed CentralGoogle Scholar
- Mammucari C, Schiaffino S, Sandri M. Downstream of Akt: FoxO3 and mTOR in the regulation of autophagy in skeletal muscle. Autophagy. 2008;4:524–6.View ArticlePubMedGoogle Scholar
- Tinsley GM, Forsse JS, Butler NK, Paoli A, Bane AA, La Bounty PM, Morgan GB, Grandjean PW. Time-restricted feeding in young men performing resistance training: A randomized controlled trial. Eur J Sport Sci. 2016:1–8.Google Scholar
- Stote KS, Baer DJ, Spears K, Paul DR, Harris GK, Rumpler WV, Strycula P, Najjar SS, Ferrucci L, Ingram DK, et al. A controlled trial of reduced meal frequency without caloric restriction in healthy, normal-weight, middle-aged adults. Am J Clin Nutr. 2007;85:981–8.PubMedPubMed CentralGoogle Scholar
- Toeller M, Buyken A, Heitkamp G, Milne R, Klischan A, Gries FA. Repeatability of three-day dietary records in the EURODIAB IDDM Complications Study. Eur J Clin Nutr. 1997;51:74–80.View ArticlePubMedGoogle Scholar
- Schroder H, Covas MI, Marrugat J, Vila J, Pena A, Alcantara M, Masia R. Use of a three-day estimated food record, a 72-hour recall and a food-frequency questionnaire for dietary assessment in a Mediterranean Spanish population. Clin Nutr. 2001;20:429–37.View ArticlePubMedGoogle Scholar
- Turconi G, Bazzano R, Roggi C, Cena H. Reliability and relative validity of a quantitative food-frequency questionnaire for use among adults in Italian population. Int J Food Sci Nutr. 2010;61:846–62.View ArticlePubMedGoogle Scholar
- Paoli A, Grimaldi K, D’Agostino D, Cenci L, Moro T, Bianco A, Palma A. Ketogenic diet does not affect strength performance in elite artistic gymnasts. J Int Soc Sports Nutr. 2012;9:34.View ArticlePubMedPubMed CentralGoogle Scholar
- Willoughby DS, Stout JR, Wilborn CD. Effects of resistance training and protein plus amino acid supplementation on muscle anabolism, mass, and strength. Amino Acids. 2007;32:467–77.View ArticlePubMedGoogle Scholar
- Paoli A, Moro T, Marcolin G, Neri M, Bianco A, Palma A, Grimaldi K. High-Intensity Interval Resistance Training (HIRT) influences resting energy expenditure and respiratory ratio in non-dieting individuals. J Transl Med. 2012;10:237.View ArticlePubMedPubMed CentralGoogle Scholar
- Lohman TG, Roche AF, Martorell R. Anthropometric standardization reference manual. Champaign: Human Kinetics Books; 1991.Google Scholar
- Heyward V. ASEP methods recommendation: body composition assessment. J Exerc Physiol. 2001;4:1–12.Google Scholar
- Pacelli QF, Paoli A, Zolesi V, Norfini A, Donati A, Reggiani C. Implementation and ground validation of a facility for functional and structural analysis of proximal upper limb muscles in microgravity. Basic Appl Myol. 2009;19:77–85.Google Scholar
- Paoli A, Pacelli QF, Cancellara P, Toniolo L, Moro T, Canato M, Miotti D, Reggiani C: Myosin isoforms and contractile properties of single fibers of human latissimus dorsi muscle. BioMed Res Int. 2013, in press.Google Scholar
- Paoli A, Pacelli QF, Neri M, Toniolo L, Cancellara P, Canato M, Moro T, Quadrelli M, Morra A, Faggian D, et al. Protein supplementation increases postexercise plasma myostatin concentration after 8 weeks of resistance training in young physically active subjects. J Med Food. 2015;18:137–43.View ArticlePubMedPubMed CentralGoogle Scholar
- Weir JB. New methods for calculating metabolic rate with special reference to protein metabolism. J Physiol. 1949;109:1–9.View ArticlePubMedPubMed CentralGoogle Scholar
- Alessandro R, Gerardo B, Alessandra L, Lorenzo C, Andrea P, Keith G, Yang Z, Antonio P. Effects of twenty days of the ketogenic diet on metabolic and respiratory parameters in healthy subjects. Lung. 2015;193:939–45.View ArticlePubMedGoogle Scholar
- Hunter GR, Seelhorst D, Snyder S. Comparison of metabolic and heart rate responses to super slow vs. traditional resistance training. J Strength Cond Res. 2003;17:76–81.PubMedGoogle Scholar
- Seo DI, Kim E, Fahs CA, Rossow L, Young K, Ferguson SL, Thiebaud R, Sherk VD, Loenneke JP, Kim D, et al. Reliability of the one-repetition maximum test based on muscle group and gender. J Sports Sci Med. 2012;11:221–5.PubMedPubMed CentralGoogle Scholar
- Varady KA, Bhutani S, Klempel MC, Kroeger CM, Trepanowski JF, Haus JM, Hoddy KK, Calvo Y. Alternate day fasting for weight loss in normal weight and overweight subjects: a randomized controlled trial. Nutr J. 2013;12:146.View ArticlePubMedPubMed CentralGoogle Scholar
- Klempel MC, Kroeger CM, Norkeviciute E, Goslawski M, Phillips SA, Varady KA. Benefit of a low-fat over high-fat diet on vascular health during alternate day fasting. Nutr Diabetes. 2013;3:e71.View ArticlePubMedPubMed CentralGoogle Scholar
- Klempel MC, Kroeger CM, Varady KA. Alternate day fasting (ADF) with a high-fat diet produces similar weight loss and cardio-protection as ADF with a low-fat diet. Metabolism. 2013;62:137–43.View ArticlePubMedGoogle Scholar
- Varady KA, Roohk DJ, Loe YC, McEvoy-Hein BK, Hellerstein MK. Effects of modified alternate-day fasting regimens on adipocyte size, triglyceride metabolism, and plasma adiponectin levels in mice. J Lipid Res. 2007;48:2212–9.View ArticlePubMedGoogle Scholar
- Kroeger CM, Klempel MC, Bhutani S, Trepanowski JF, Tangney CC, Varady KA. Improvement in coronary heart disease risk factors during an intermittent fasting/calorie restriction regimen: relationship to adipokine modulations. Nutr Metab. 2012;9:98.View ArticleGoogle Scholar
- Bhutani S, Klempel MC, Berger RA, Varady KA. Improvements in coronary heart disease risk indicators by alternate-day fasting involve adipose tissue modulations. Obesity. 2010;18:2152–9.View ArticlePubMedGoogle Scholar
- Gulcelik NE, Halil M, Ariogul S, Usman A. Adipocytokines and aging: adiponectin and leptin. Minerva Endocrinol. 2013;38:203–10.PubMedGoogle Scholar
- Mansell PI, Fellows IW, Macdonald IA. Enhanced thermogenic response to epinephrine after 48-h starvation in humans. Am J Physiol. 1990;258:R87–93.PubMedGoogle Scholar
- Zauner C, Schneeweiss B, Kranz A, Madl C, Ratheiser K, Kramer L, Roth E, Schneider B, Lenz K. Resting energy expenditure in short-term starvation is increased as a result of an increase in serum norepinephrine. Am J Clin Nutr. 2000;71:1511–5.PubMedGoogle Scholar
- Cangemi R, Friedmann AJ, Holloszy JO, Fontana L. Long-term effects of calorie restriction on serum sex-hormone concentrations in men. Aging Cell. 2010;9:236–42.View ArticlePubMedPubMed CentralGoogle Scholar
- Kumar S, Kaur G. Intermittent fasting dietary restriction regimen negatively influences reproduction in young rats: a study of hypothalamo-hypophysial-gonadal axis. PLoS ONE. 2013;8:e52416.View ArticlePubMedPubMed CentralGoogle Scholar
- Paoli A, Bosco G, Camporesi EM, Mangar D. Ketosis, ketogenic diet and food intake control: a complex relationship. Front Psychol. 2015;6:27.View ArticlePubMedPubMed CentralGoogle Scholar
- Belobrajdic DP, Frystyk J, Jeyaratnaganthan N, Espelund U, Flyvbjerg A, Clifton PM, Noakes M. Moderate energy restriction-induced weight loss affects circulating IGF levels independent of dietary composition. Eur J Endocrinol. 2010;162:1075–82.View ArticlePubMedGoogle Scholar
- Fontana L, Villareal DT, Das SK, Smith SR, Meydani SN, Pittas AG, Klein S, Bhapkar M, Rochon J, Ravussin E, et al. Effects of 2-year calorie restriction on circulating levels of IGF-1, IGF-binding proteins and cortisol in nonobese men and women: a randomized clinical trial. Aging Cell. 2016;15:22–7.View ArticlePubMedGoogle Scholar
- Tipton KD, Rasmussen BB, Miller SL, Wolf SE, Owens-Stovall SK, Petrini BE, Wolfe RR. Timing of amino acid-carbohydrate ingestion alters anabolic response of muscle to resistance exercise. Am J Physiol Endocrinol Metab. 2001;281:E197–206.PubMedGoogle Scholar
- Tipton KD, Elliott TA, Cree MG, Aarsland AA, Sanford AP, Wolfe RR. Stimulation of net muscle protein synthesis by whey protein ingestion before and after exercise. Am J Physiol Endocrinol Metab. 2007;292:E71–6.View ArticlePubMedGoogle Scholar
- Cnop M, Havel PJ, Utzschneider KM, Carr DB, Sinha MK, Boyko EJ, Retzlaff BM, Knopp RH, Brunzell JD, Kahn SE. Relationship of adiponectin to body fat distribution, insulin sensitivity and plasma lipoproteins: evidence for independent roles of age and sex. Diabetologia. 2003;46:459–69.PubMedGoogle Scholar
- Higashiura K, Ura N, Ohata J, Togashi N, Takagi S, Saitoh S, Murakami H, Takagawa Y, Shimamoto K. Correlations of adiponectin level with insulin resistance and atherosclerosis in Japanese male populations. Clin Endocrinol. 2004;61:753–9.View ArticleGoogle Scholar
- Khodabandehloo H, Gorgani-Firuzjaee S, Panahi G, Meshkani R. Molecular and cellular mechanisms linking inflammation to insulin resistance and beta-cell dysfunction. Transl Res. 2016;167:228–56.View ArticlePubMedGoogle Scholar
- Halberg N, Henriksen M, Soderhamn N, Stallknecht B, Ploug T, Schjerling P, Dela F. Effect of intermittent fasting and refeeding on insulin action in healthy men. J Appl Physiol. 1985;2005(99):2128–36.Google Scholar
- Seidell JC, Muller DC, Sorkin JD, Andres R. Fasting respiratory exchange ratio and resting metabolic rate as predictors of weight gain: the Baltimore Longitudinal Study on Aging. Int J Obes Relat Metab Disord. 1992;16:667–74.PubMedGoogle Scholar
- Fontana L, Weiss EP, Villareal DT, Klein S, Holloszy JO. Long-term effects of calorie or protein restriction on serum IGF-1 and IGFBP-3 concentration in humans. Aging Cell. 2008;7:681–7.View ArticlePubMedPubMed CentralGoogle Scholar
- Anisimov VN. Insulin/IGF-1 signaling pathway driving aging and cancer as a target for pharmacological intervention. Exp Gerontol. 2003;38:1041–9.View ArticlePubMedGoogle Scholar
- Vainshtein A, Grumati P, Sandri M, Bonaldo P. Skeletal muscle, autophagy, and physical activity: the menage a trois of metabolic regulation in health and disease. J Mol Med. 2014;92:127–37.View ArticlePubMedGoogle Scholar
- Fujita S, Dreyer HC, Drummond MJ, Glynn EL, Volpi E, Rasmussen BB. Essential amino acid and carbohydrate ingestion before resistance exercise does not enhance postexercise muscle protein synthesis. J Appl Physiol. 1985;2009(106):1730–9.Google Scholar
- Burke LM, Hawley JA, Ross ML, Moore DR, Phillips SM, Slater GR, Stellingwerff T, Tipton KD, Garnham AP, Coffey VG. Preexercise aminoacidemia and muscle protein synthesis after resistance exercise. Med Sci Sports Exerc. 2012;44:1968–77.View ArticlePubMedGoogle Scholar








